For many patients in Oceanside and on the South Shore of Long Island, the journey through sciatica begins with a familiar hope: that rest, physical therapy, or perhaps a round of anti-inflammatory medication will resolve the sharp, radiating pain traveling from the lower back down the leg. However, when these conservative measures fail to provide lasting relief, the conversation often shifts toward more advanced clinical interventions like spinal cord stimulation.
At Mosaic Pain, led by Dr. Brian Singer, we prioritize a patient-centric approach to recovery. We understand that by the time a patient reaches our office, they are often weary of the “medical treadmill” and are looking for a definitive path forward. One such path for chronic, treatment-resistant sciatica is Spinal Cord Stimulation (SCS).
Understanding the Clinical Transition
Sciatica is not a diagnosis in itself, but a symptom of an underlying issue—often a herniated disc or spinal stenosis—compressing the sciatic nerve. When the resulting nerve pain becomes chronic, it can alter the way the nervous system processes pain signals.
Before considering a permanent surgical intervention, our practice often explores targeted interventional treatments. For instance, in cases where the pain mechanics involve the lower pelvis and base of the spine, Sacroiliac joint injections can be a vital diagnostic and therapeutic tool. By utilizing Sacroiliac joint injections, we can pinpoint whether the SI joint is a primary contributor to the patient’s discomfort, ensuring that we aren’t overlooking localized issues before moving toward neuromodulation.
How Spinal Cord Stimulation Works
If interventional options like Sacroiliac joint injections or epidural blocks have provided only temporary reprieve, Spinal Cord Stimulation may be the logical next step.
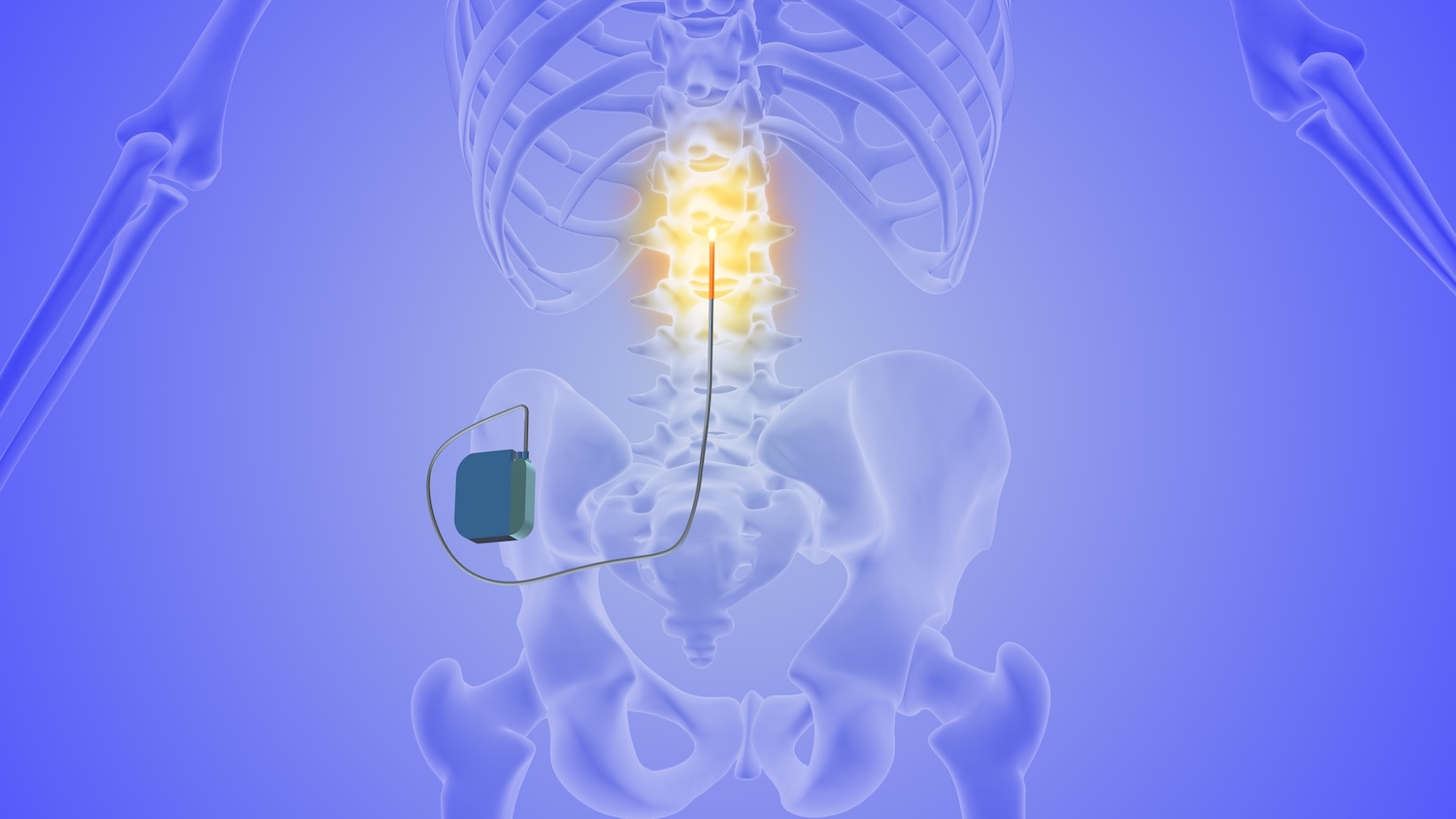
SCS involves a small device, similar to a pacemaker, that delivers low-level electrical impulses to the spinal cord. These impulses interrupt the pain signals before they reach the brain, replacing the sharp “electric” sensation of sciatica with a mild, often unnoticeable sensation.
What makes this a “human-first” technology is the trial phase. Unlike irreversible surgeries, SCS allows the patient to “test drive” the system for several days. This ensures that the patient feels a significant improvement in their daily mobility and quality of life before a long-term commitment is made.
A Partnership in Advocacy
Navigating the aftermath of a hospital stay or a failed surgery is physically and administratively taxing. Dr. Brian Singer and the team at Mosaic Pain act as your advocates in this process. We focus on clinical precision, ensuring that every patient understands the “why” behind their treatment.
Whether we are administering Sacroiliac joint injections to calm localized inflammation or programming an SCS device for long-term nerve modulation, the goal remains the same: a return to functional independence. We pride ourselves on being a board-certified, independent alternative to the high-volume hospital environment, offering a more personal level of care for the Oceanside community.
Schedule a consultation at Mosaic Pain today, and let’s find the pain management approach that fits you.